Let me preface this post by noting that I am not a medical expert, nor have I ever played one on TV.
I am, however, a Type 1 diabetic, and I’ve been that way for the last fifteen years.
I’ve fought my way through it and come to the realization that it’s not a battle I can win—it’s just a battle that I have to keep fighting.
There is no day off from diabetes, no vacation you can take. I tried that once and ended up in an emergency room on Christmas Eve. After that four-day hospital stay, dark purple bruises covered my arms for a week, and I knew I had to make changes. But it took time and a number of serious events to bring me to that point.
For years following my diagnosis, I was on top of things—too on top of things based on what my doctor told me. I believed in keeping my number as close to normal as possible, which meant that I kept my number lower than a diabetic should. I would experience shakes and moments of incoherence as a result.
On the opposite end of the spectrum, I’ve also experienced high blood sugar. My eyes have blurred, and I’ve felt sluggish. I’ve known frustration as others have been able to eat and drink around me, while I would have to wait for my shot to kick in.
Because that’s how I eat as a diabetic—I take a shot.
I’ve contemplated on more than one occasion whether eating is worth it, because do I really want to take another shot?
Thankfully, I’ve talked myself out of those low moments in my life, but it is one more part of the struggle.
In the end, though, I know my life is worth it, which means I eat, take five shots a day, and keep on enjoying my existence.
I do restrain myself, though. I’ve only had sips of regular soda during my time as a T1D—and that was only when I was experiencing hypoglycemia. But that doesn’t mean I don’t have a bite of cake or a piece of chocolate here or there. I just do so in moderation.
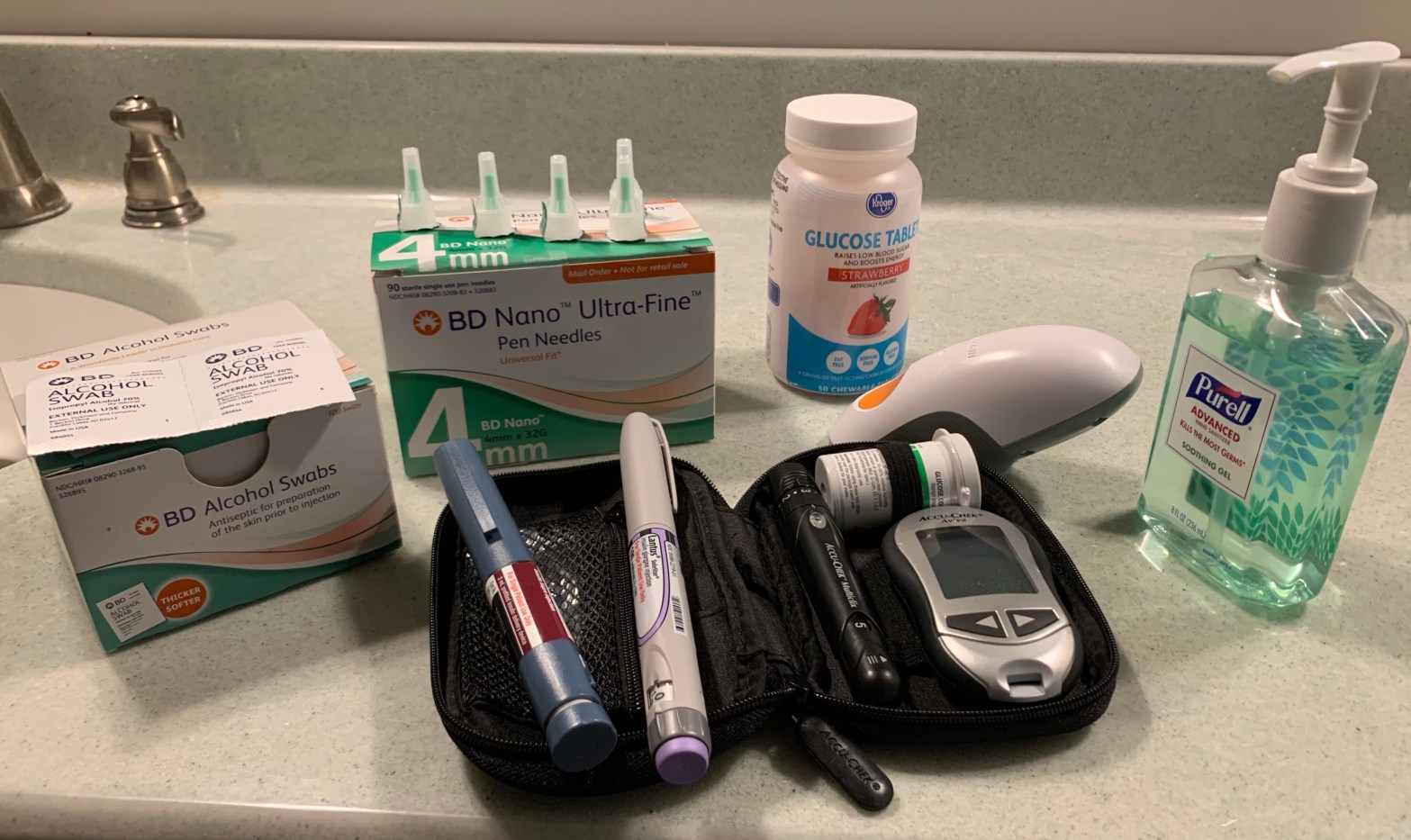
And for years, I managed my diabetes outside of myself. I carried a large purse with all my supplies—two types of insulin pens, needles, alcohol swabs, a glucose meter, test strips, a finger poker, glucose tablets—in addition to everything else a normal person carries in their purse.
And I made it work.
I kept my A1c below 6.0 for a long time, but then I had setbacks.
The hardest was my mother’s passing. It was unexpected and painful. She was my advocate and my support system. She was there as the doctors explained to 20-year-old me that I would need to take shots everyday for the rest of my life. She took me to a nutritionist to figure out what I should be eating. And she learned to administer my shots and watch out for the signs of low blood sugar just in case.
And then she was gone. She’d lived a healthy lifestyle, but that didn’t stop the tragedy of her passing.
This was a difficult moment for me in so many ways, and I can’t cover them all here. In terms of my diabetes though, after I lost her, I wasn’t as careful as I should have been. I questioned what the point was. If someone healthy could pass away like that, why should I bother with my daily health struggles? Why shouldn’t I just wing it?
That attitude led to serious lows—to the point where ambulances had to be called, and I spent my first night in a hospital.
It took time, but I pushed myself back into my diabetes management when I realized I couldn’t keep going like I was.
But like I said, diabetes isn’t a battle you can win—it’s a constant fight, and that means time and effort without pause.
Fast forward a few years, I was in a new job with a new house, and taking on challenges and opportunities as fast as they showed up at my door. I couldn’t keep up with the pace and the stress, and something had to give.
Sadly, it was my diabetes care. I wanted to enjoy life the same way other people were around me. Besides, I told myself, I’d had diabetes for years. I could skip a few finger pricks and just go on my instincts alone.
Unfortunately, I wasn’t as skilled as I thought.
A few months after starting a new relationship with a wonderful man—on the night where I supposed to meet his mother—I couldn’t stop throwing up. In the rush of everything, I’d left my glucose meter at home, so I didn’t know how to react—insulin or food? I didn’t know if I was experiencing low blood sugar, which sometimes makes me nauseous, or something else.
I ended up going to the hospital that night instead of dinner.
My boyfriend drove me and stayed the night at the ER with me.
That was Christmas Eve. Christmas Day was spent in the hospital receiving IV insulin and antibiotics. Somewhere along the way, I’d caught an infection, and if I’d been watching my blood sugar, I would have seen my body was fighting something. My number always shoots up when I have something in my system.
But I’d been too busy to care about my health.
After several days in the hospital, my priorities shifted. I knew I couldn’t keep living like this, and that I needed to once again stay on top of my diabetes.
But I didn’t know if I had the dedication I’d had in my 20’s. Sustaining an A1c below 6.0 wasn’t easy, and I had more responsibilities in my life and my job. Despite these obstacles, I decided I wasn’t going to just give up.
I wanted a healthy lifestyle, so I went back to poking my fingers four times a day—no matter how much my typing fingers might protest.
And luckily, I had help.
My boyfriend was always encouraging, always asking me questions. And it was nice to have a partner in this fight.
But one problem is that diabetes isn’t an exact science. How something impacts you today may not be the same way it will impact you tomorrow, and I couldn’t stop my habit of wanting my blood sugar to be lower rather than higher.
Several times, my boyfriend had frightening experiences where he couldn’t wake me easily or if I was able to wake, I wasn’t coherent. I don’t fully remember these episodes, but I know he won’t forget them.
I’m stubborn during low blood sugar moments, and a finger poke often isn’t something I’m willing to do in that state.
After those instances, my boyfriend and I had several long conversations about my care going forward.
I wanted to keep my diabetes separate from my person—so no needles, tubes, or anything else attached to my skin for any extended period of time. But it was clear, having my glucose meter unusable at a moment where it was needed wasn’t a solution either.
I knew my boyfriend meant well in suggesting a continuous glucose monitor, but I just didn’t want to hear it.
I met with people—other diabetics who had a monitor. I saw their devices, attached to their skin, and listened to their stories.
So did my boyfriend. He asked people questions and kept leaving reminders for me about what he learned. After months together, and one more low episode, we talked, and I was convinced to try it.
What did I have to lose? If it was horrible, I was determined to rip the thing off and be done with it.
So the kit arrived, and with my boyfriend cheering me on, the first sensor of my continuous glucose monitor was on my skin.
I won’t lie—tears were shed.
Not because of physical pain—there was slight discomfort initially, but nothing unmanageable.
I cried because it marked a change in my life. I had kept a distance between myself and my diabetes, but that wasn’t going to be the case so long as this device was on my skin. It would be on me constantly, never giving me a moment’s peace from my diabetes.
And two hours later, once the device finished its warmup, I saw my blood sugar appear on my phone for the first time. I was also able to share that number with my boyfriend’s phone, and both of us would receive alerts if my blood sugar approached serious levels.
These were appealing features. A regular glucose meter can only tell you your blood sugar as of a point in time, but it doesn’t tell you what direction things are heading.
The new device provides my number and its direction, meaning I have that much more knowledge to use in my constant battle—all without further damage to my fingertips.
Yes, I do still test using my old meter—to verify or calibrate my continuous glucose monitor or if something goes wrong, but it’s no longer daily.
And the writer in me is grateful. My fingers used to sting after testing, so typing wasn’t as fun. But now, my fingers rarely have to go through that pain.
On top of that, I know my blood sugar every five minutes, and I can see in real-time how foods impact me. It helps me plan meals—and enjoy them. I also have an app that lets me know a projection of my A1c.
I’ve learned many lessons during the two years I’ve now been using a continuous glucose monitor and my fifteen years of diabetes.
1) Know what makes the battle easier.
For me, that’s a support system. I was lucky to have my mother at the start of my journey, and I’m lucky to have my boyfriend-now-husband as my partner in this battle today. They helped me through several difficult decisions related to my diabetes, and they made the struggle more bearable.
2) Education is empowering.
Not only have I spent time reading, researching, and testing how to handle my diabetes, I also believe in letting others know about my health. I’ve never been shy in sharing information about my diagnosis, and it’s helped me and others to live better. Finding forums where other diabetics discuss their experiences has been insightful as well, and it’s reminded me that others share the same challenges.
I’ve also learned that educating the people directly around you can be a helpful tool in dealing with diabetes. Having my boss and coworkers know that I’m diabetic means they don’t push me to eat things I shouldn’t and they’re also understanding if I have to eat in front of them.
3) Find what works for you and then follow through with it.
Again, I’m not a medical professional. I can only speak to my own T1D journey and what I’ve heard from others. One thing seems pretty certain, though—no two people have the exact same situation in terms of diabetes. What works for me may not work for others, but I know I’ve benefitted from listening to others. I didn’t want to hear about a continuous glucose monitor for my first thirteen years as a diabetic, but circumstances changed for me. And once I gave it a try, I found the monitor made a number of things in my life easier—but only because I’m sticking with it. Every ten days, I install a new sensor—needle through the skin and strong adhesive holding on tightly, but it means warnings about highs and lows, better knowledge of where I stand at any given moment, and fewer finger sticks.
4) Finding something that works doesn’t mean the battle is over.
Yes, I believe my continuous glucose monitor is helping me. It’s keeping me safe from my low habits, and helping me to prevent highs, but I’m still diabetic. I still require insulin injections in order to survive. I still have to be careful about what I eat. I still have to exercise, go to the doctor, and do all the things that everyone should be doing for their health—but as a diabetic, I seem to have to do them to an extreme degree. I still can’t take a break from diabetes. Each day the battle continues. With the monitor, though, I can see the results of the battle in real time, and occasionally I feel like those readings provide me with a win.
At the end of the day, I keep fighting, I keep reading, and I keep writing. I enjoy my life too much to let this battle tear me down. I may still have a bad moment here and there, but I’m not giving up.
I’m still optimistic that one day there might be a cure or a needle-free way to read blood sugar (even if my cynical side tries to convince me otherwise from time to time). But until then, I’m keeping the device on my arm and hope in my heart.
And to any diabetic out there who reads this, know you’re not alone in this fight.
Take care of yourself, and take care of each other.
~
© Virginia Gale, The Glass Is Half Shattered, and virginiagale.com, 2021. Unauthorized use and/or duplication of this material without express and written permission from this site’s author and owner is strictly prohibited.